In 2017, the typical employer healthcare costs will be $15,259 for an insurance plan for a family of four, or 57% of the total cost. The employee will bear about 43% of the cost, or $11,685, typically paid via payroll deduction or point-of-service cost sharing. The total healthcare cost will be an employer sponsored insurance plan for a typical American family of four is $26,944.
This data is courtesy of the Milliman Medical Index, an annual report issued by global consulting and actuarial firm Milliman, Inc. The firm has been tracking health care costs since 2001, and is unique among health cost studies because “it measures the total cost of healthcare services used by the family of four, including out-of-pocket expenses paid at time of service.”
Study authors note that although there is a record-low 4.3% cost increase, it is still an increase of more than $1100 for a typical family of four. See the trend lines over recent years:
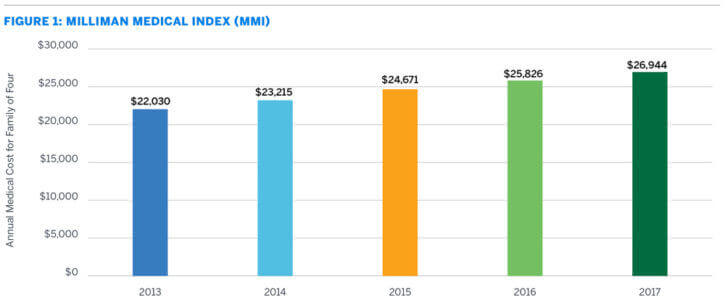
One question that many employers have is whether healthcare reform – such as ACA and AHCA – will help mitigate costs. The report addresses this:
Some stakeholders have held out hope that federal healthcare reform efforts would help control healthcare cost growth. So far, those efforts have had relatively little direct impact on the MMI, because the MMI represents healthcare costs in an employer-sponsored health plan, while the primary focus of healthcare reform has been on the individual insurance marketplace and Medicaid. The employer market tends to be one of the most stable markets for health insurance companies, and one of the most financially important for healthcare providers such as hospitals and physicians.
What employers can do do to reduce healthcare costs
Corporate wellness programs bolstered by incentives can help employees improve overall health by focusing on so-called “lifestyle diseases” that are the result of poor health habits – poor diet, lack of exercise, smoking, substance abuse, and stress. Wellness programs can deliver $3 return for every $1 invested in improving workers’ health; some programs have reduced health costs by 18%, and up to 28% for older workers.
The problem for many employers is that benefit budgets are strapped and wellness programs get deferred due cost. But there are many ways to structure incentives so that wellness programs can be nearly revenue neutral. In the Affordable Care Act, one key provision enables employers to offer wellness program participants deeper financial incentives associated with their employee contributions to the cost of health insurance. That means that non-participanting employees can now be charged up to an additional 30% of the total health insurance cost; In the case of smoking, the allowable incentive grows to 50%. Explore ways to structure incentives and plan wellness programs that will yield results in our TotalCare Wellness Knowledge Center.

